Acne Vulgaris: Acne vulgaris is a chronic skin disease of the pilosebaceous unit and develops due to blockages in the skin’s hair follicles. These blockages are thought to occur as a result of the following four abnormal processes: a higher than normal amount of sebum production (influenced by androgens), excessive deposition of the protein keratin leading to comedone formation, colonization of the follicle by Propionibacterium acnes bacteria, and the local release of pro-inflammatory chemicals in the skin.
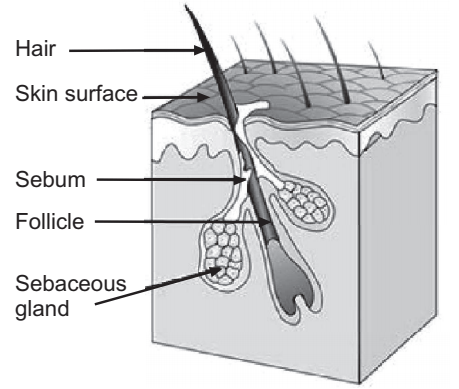
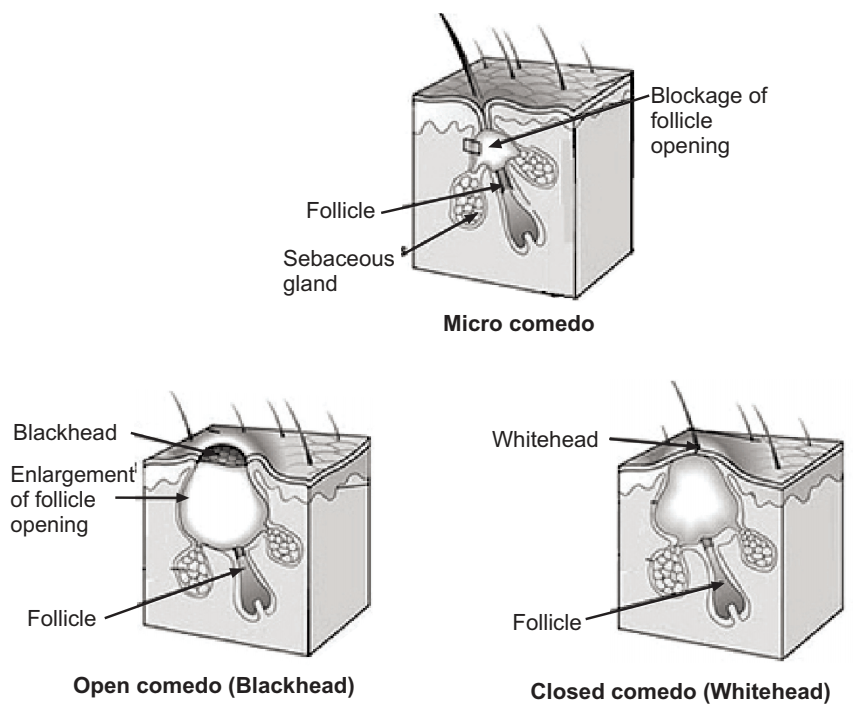
The earliest pathologic change is the formation of a plug (a microcomedone), which is driven primarily by the excessive proliferation of keratinocytes in the hair follicle. In normal skin, the skin cells that have died come up to the surface and exit the pore of the hair follicle. However, increased production of oily sebum in those with acne causes the dead skin cells to stick together. The accumulation of dead skin cell debris and oily sebum blocks the pores of the hair follicle, thus forming the microcomedone. This is further exacerbated by the biofilm created by P. acnes within the hair follicle. If the microcomedone is superficial within the hair follicle, the skin pigment melanin is exposed to air, resulting in its oxidation and dark appearance (known as a blackhead or open comedone). In contrast, if the microcomedone occurs deep within the hair follicle, this causes the formation of a whitehead (known as a closed comedone). Other troublesome acne lesions can develop, including the following:
- Papules: Inflamed lesions that usually appear as small, pink bumps on the skin and can be tender to the touch.
- Pustules (pimples): Papules topped by white or yellow pus-filled lesions that may be read at the base.
- Nodules: Large, painful, solid lesions that are lodged deep within the skin.
- Cysts: Deep, painful, pus-filled lesions that can cause scarring.
In a sebum-rich skin environment, the naturally occurring and largely commensal skin bacterium P. acnes readily grow and can cause inflammation within and around the follicle due to activation of the innate immune system. P. acnes triggers skin inflammation in acne by increasing the production of several pro-inflammatory chemical signals known to be essential to Comedone formation. P. acnes is also capable of provoking additional skin inflammation by altering sebum’s fatty composition. The inflammatory properties of P. acnes can be further explained by the bacterium’s ability to convert sebum triglycerides to pro-inflammatory free fatty acids via secretion of the enzyme lipase. This inflammatory cascade typically leads to the formation of inflammatory acne lesions, including papules, infected pustules, or nodules. If the inflammatory reaction is severe, the follicle can break into the deeper layers of the dermis and subcutaneous tissue and cause the formation of deep nodules.
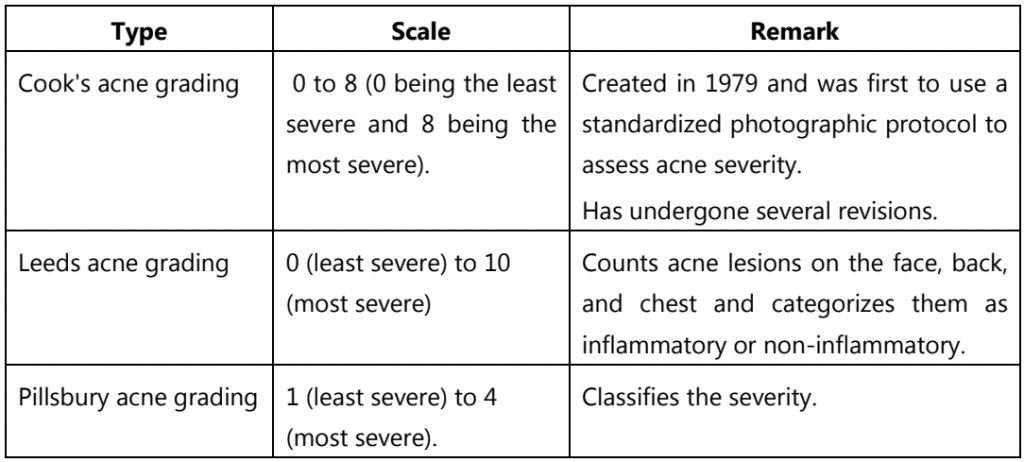
Historical and physical clues that may suggest hormone-sensitive acne include onset between ages 20 and 30; worsening the week before a woman’s menstrual cycle; acne lesions predominantly over the jawline and chin; and inflammatory/nodular acne lesions. Several scales (See Table.1) exist to grade the severity of acne vulgaris, but no single technique has been universally accepted as the diagnostic standard.
Table.1
Cosmetics/ Treatment of Acne Vulgaris
The acne treatment prescribed or recommended by a dermatologist may contain drying ingredients like benzoyl peroxide, which can suck the moisture from the skin and leave it looking red and irritated. A good moisturizer will retain the water in the skin and help avoid unsightly drying and peeling. In reality, moisturizers are an essential part of the acne skin care routine. A lightweight, oil-free moisturizer labeled “non-comedogenic” (which won’t clog pores) containing glycerin and hyaluronic acid holds moisture in the skin. Greasy products that contain pimple-producing ingredients such as cocoa butter, mineral oil, or cold cream should be avoided.
Make sure you also check our other amazing Article on : Wrinkles
